When you go to the hospital in an emergency situation, the last thing on your mind is probably your patient status. But whether you are classified as an “outpatient” or as an “inpatient” can make a huge difference in what you are expected to pay for your visit, especially as a Medicare beneficiary, since it will determine whether Part A or Part B will help pay the costs. Knowing the rules of these classifications, though, can help you to avoid getting a large and unexpected bill in the mail.
Outpatient Status Explained
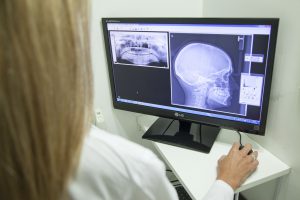
In some cases, you might go to the emergency room, get lab tests, an X-ray, MRI, or other procedures, but not get admitted to the hospital. If this happens, you will be considered an outpatient, or as an observation stay. You can be considered an outpatient even if you stay overnight at the hospital; for example, if you have an outpatient procedure and are kept overnight to be monitored, you are still under outpatient care, unless you are admitted under a doctor’s orders.
Outpatient Medicare Coverage
Medicare Part B will pay for any medical care that is performed under outpatient status, including diagnostic imaging tests, emergency room visits, medical observation, outpatient surgery, lab tests, x-rays, and colonoscopies. Remember, though, that Medicare Part B will only cover 80% of the cost of these qualified expenses, leaving you to pay your 20% coinsurance after meeting your Part B deductible.
Inpatient Status Explained
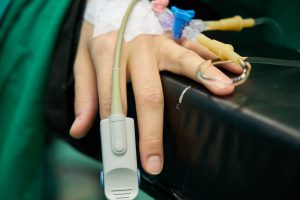
After getting assessed as an outpatient at the hospital, you could get admitted to the hospital under a doctor’s order – then, and only then, will your status change to that of an inpatient. Any care you continue to get after this will be considered on an inpatient basis until you are discharged.
Inpatient Medicare Coverage
Medicare Part A completely covers any medical care that is on an inpatient basis, so you will not have to pay any coinsurance (as long as your stay is under 60 days). The only thing you will be responsible for is your Medicare Part A deductible and a daily coinsurance if your hospital stay goes beyond 60 days. In addition, if your stay lasts longer than 90 days, you will have an even higher coinsurance to pay.
Skilled Nursing Facility Coverage
These two classifications can become confusing, and even problematic, if you get transferred to a skilled nursing facility directly from the hospital. If you are still considered an outpatient, or under an observation stay, when you are transferred, Medicare will not cover your stay at the facility. In order for Medicare to cover a stay at a skilled nursing facility, you will have to be admitted to the hospital and considered an inpatient for 3 days prior to the transfer. 
How to Save on Medical Expenses
If you’d like to save money on your medical expenses, the best way to do so is by considering a Medicare Supplement Plan. Part A might cover inpatient hospital care almost completely, but you’ll probably find that you’ll end up using Medicare Part B far more, since it covers most everyday and outpatient services – and Part B only covers 80% of medical expenses! That remaining 20% can really add up, but a Medicare Supplement Plan can help cover these costs. Each plan offers different coverage at different price points, so you’re sure to find one that meets your individual needs. Not sure where to begin? EZ can compare the 10 different Medicare Supplement Plans and provide you with quotes as well as guidance as to which will provide you the most coverage with the most savings. To get free quotes, simply enter your zip code in the bar above, or to speak to a licensed agent, call 888-753-7207. No obligation.