When you think of plastic surgery, the Kardashians or a Real Housewife of some random city probably come to mind, but what they’ve actually had is cosmetic surgery. There is a difference between the 2 and if you have Medicare, the good news is one of them may be covered.
Plastic Surgery vs. Cosmetic Surgery

Plastic surgery is a procedure performed because it’s medically necessary. That means you need it for medical reasons to improve the health or function of your body. Plastic surgery is sometimes referred to as reconstructive surgery. You may need plastic surgery for medical reasons after an accident, infection, tumor, malformation of a body party or other disease, such as breast cancer. Some examples of medically necessary plastic surgery covered by Medicare include treatment for severe burns, facial reconstruction following a car accident, or a breast reconstruction after a partial or full mastectomy. Cosmetic surgery is a type of plastic surgery used to enhance the natural features of the body. Surgeons generally perform cosmetic surgery to reshape normal structures of the body to improve your appearance or enhance your self-esteem. These are generally not covered by Medicare. If you’re looking to get a breast lift, facelift, neck lift, or chemical peels covered, you’re out of luck because those are considered cosmetic and are not medically necessary.
Cosmetic Surgery for Medical Reasons

Medicare may pay for a cosmetic surgery if you need it for medical reasons but you must obtain prior authorization. This means your doctor must send a prior authorization request to Medicare for approval before performing the procedure. If Medicare approves the request, you’ll pay your Medicare Part A and/or B deductible and coinsurance costs, depending on the setting of your plastic surgery, such as inpatient or outpatient. Some examples of cosmetic surgeries that may be considered medically necessary are botox to treat muscle disorders or a nose job to correct structural nose defects that affect your breathing. An eyelid surgery to remove excess tissue around your eye that may be impairing your peripheral vision would probably qualify as medically necessary as well. Only your doctor can determine whether your procedure is medically necessary so be sure to have a thorough conversation with them before going through with a procedure.
Find a Medicare Supplement Plan
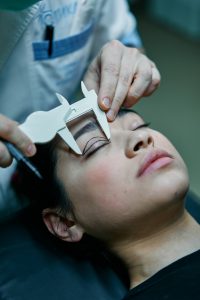
There are many reasons why you might need or want plastic surgery. Luckily Medicare Parts A and B may cover plastic surgery if you need it for medical reasons. If your plastic surgery is covered by Medicare, you may be able to find a Medicare Supplement Insurance plan that helps pay for some of your Medicare copays, deductibles and more and EZ can help. Our agents work with the top-rated insurance companies in the nation, which makes comparing plans easy, quick, and free. To get free instant quotes on plans that cover your doctors, simply enter your zip code in the bar above, or to speak to a local licensed agent, call 888-753-7207.

